At a Glance
- Many things happen as we age that makes a loss of bowel control more likely.
- Illness, injury, changes in bowel habits and other factors affect the ability to stay in control.
- Loss of bowel control is surprisingly common. It happens to a lot of people.
- There are a number of ways to be helped.
- This article will help you understand what is wrong and what you can do about it.
Continence, our control over when and where we go to the bathroom, is something most of us learn at an early age. We generally take it for granted – until something goes wrong. “Incontinence” is the word used to describe loss of this control.
Bowel incontinence occurs when the loss of control of gas, liquid stool, or solid stool is enough to cause discomfort or distress. Urinary incontinence is the loss of control of urine from the bladder. Bowel incontinence is a sign that something is wrong – some part of the bowel control system is not working as it should.
Having an episode of bowel incontinence can be very upsetting. People often feel so embarrassed when this happens to them that they do not tell anyone about it, not even their spouse or doctor.
It is common for persons who suffer this to go to lengths to hide the condition. As a result, they may stop doing many of the things they enjoy; they may experience a loss of personal freedom. They may feel many parts of their life slipping away – and they may not receive the help they need.
If you experience bowel incontinence, here are three important things to know:
- You are not alone – many people have this condition
- You do not have to just, “live with it”
- You can find help, and ways to treat and manage the condition
Causes of incontinence
Incontinence has many causes. It is not a normal part of aging, but as you age, you may be more at risk for the condition.
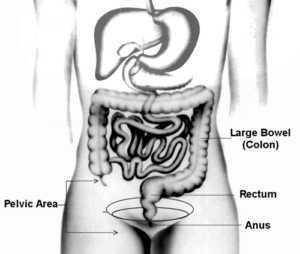 In order to maintain bowel control, the pelvic area must work correctly. If not, incontinence may occur. Injury or illness can cause a loss of normal function and bowel control. Physical limitations or disabilities, and poor general health are key factors that can play a role.
In order to maintain bowel control, the pelvic area must work correctly. If not, incontinence may occur. Injury or illness can cause a loss of normal function and bowel control. Physical limitations or disabilities, and poor general health are key factors that can play a role.
Nerves must function correctly to sense the urge to have a bowel movement or the presence of gas in the rectum. Muscles must function correctly to hold in the rectal contents.
Nerve damage that occurs in diseases like multiple sclerosis, diabetes, or stroke can play a part in incontinence. Injury, from accidents, pregnancy, or other trauma, can also damage nerves and muscles.
Conditions that strain normal function – such as diarrhea or constipation – may also cause leakage or loss of control. These are just a few examples. Clearly, many conditions that affect men and women may result in loss of bowel control.
The effect of age on continence
Diseases or injuries are not the only risks for incontinence. As you age, many physical changes will occur naturally. These changes have an effect throughout the body including on the organs, nerves, and muscles that control continence. Muscles will lose their strength, some nerves will function less well, and tissue and organs will lose some of their ability to stretch.
The bowel control system
Many things must happen in the body so that you know when you need to have a bowel movement (or pass gas) and are able to hold it in until you decide when and where to empty. The rectum is a tube shaped organ at the end of the colon that stores stool. As the rectum fills, it stretches to have room for the stool moving from the colon. You normally will feel when stool fills the rectum; you will have the sensation of the urge, or need, to have a bowel movement. Muscles around the rectum will tighten to hold in the stool.
If the muscles around the rectum are weak, you may feel a sudden and very strong urge and need to rush to the toilet. Stool may leak before you reach the toilet.
If nerves are damaged, you may not know when stool is present. The urge to have a bowel movement may not be felt and you make leak stool without even feeling it.
Seepage of stool may also occur if the muscles around the rectum do not work right. If the rectum does not stretch, it will not be able to store enough stool and incontinence can result.
What to do – talking to your doctor
If you experience bowel incontinence, the first thing to do is tell your doctor about it. Most people feel uneasy talking about their stool, intestinal gas, or bowel movements. But doctors understand that these are very normal and necessary processes in all of us.
Doctors and other therapists are there to help when bodily processes go wrong. So the first very important step is to talk plainly about the problems you are experiencing.
Begin by describing your troubling symptoms. Be specific so your doctor (or therapist) clearly understands the problem. Here are some examples:
- Diarrhea – Diarrhea is a common factor that can cause incontinence. If you are experiencing loose or runny stool that is leaking, do not simply say to your doctor that you, “have diarrhea.” That does not tell the doctor that you are losing control of the stool. Be clear, “When I have diarrhea it leaks into my clothing with little or no warning. I can’t stop it in time to get to the toilet.”
- Constipation – You may be surprised that constipation is another common factor that can lead to incontinence. Hard stool stuck in the rectum can build up to the point where watery stool leaks around it. Be sure to tell your doctor if you are constipated – not simply that you, “have leakage of loose stool.” Your doctor might naturally think you have diarrhea and prescribe a treatment that makes you even more constipated. Be clear about any changes in your bowel habit, such as ongoing constipation or diarrhea.
- Pain – Continually squeezing together the muscles around your rectum, because of fear that stool may leak, can cause the muscles to cramp and get tired. The result will be pain, which can be severe, and muscle weakness. Both will make your incontinence worse. If this is happening to you, explain it to your doctor.
Next, let your doctor know how this is affecting your daily life. Ask yourself this question, “How have my bowel control problems changed my life?” The answer, such as, “I’m afraid to leave my house” or “I don’t socialize anymore” is important information for your doctor.
These kinds of changes may have come on gradually. They are important for you to recognize. This is your own personal test of how serious your disorder is. How often you experience incontinence is not always as important as how the problem has changed your life. A goal of your treatment will be to help you get back, as much as possible, the parts of your life that have been lost because of incontinence.
If you have lost sensation, you may have no feeling of the urge to pass gas or stool. Knowing you may experience incontinence with no warning, at any time, may mean that you are worried about it all the time. This can be a heavy burden that takes a toll on daily life. Be sure to explain this to your doctor as well.
Your doctor will want to know how long you have been experiencing episodes of incontinence and if it has been getting worse or has changed over time. Other things to tell your doctor about include:
- Any other illnesses that may be affecting your health
- A list of all medicines you are taking, including
- Prescription and over-the-counter
- Herbal supplements
- Vitamins or mineral supplements
- How much and how often you take any of these
- Any surgeries you have ever had in the past
If you are a woman who has given birth, even many years ago, let your doctor know. Tell your doctor:
- How many children you had by vaginal delivery
- How many hours you were in labor
- If you had an episiotomy (a cut the doctor sometimes makes in the vaginal area)
- If forceps were used
- If you had any tearing that needed surgical repair
Any of these factors could play a part in damage to nerves and muscles, which then get weaker or less able to do their job with age. The resulting problems affecting continence may take 20 or more years to show up.
Your doctor may want to run tests before coming up with a treatment plan. Various tests can look at how well the organs, muscles, and nerves that affect your continence are working. They can also look for signs of disease or injury. The doctor should explain to you the reason for the test. You should also understand what to expect during and after the test. If you do not understand something, be sure to ask.
Treating bowel incontinence
The goal of treatment is to improve function – both in your body and in your daily life. Ways to eliminate or reduce symptoms may involve changes in what you eat, bowel retraining, therapy to change the way nerves or muscles respond, surgery, or other therapies.
You can learn strategies that help you manage the symptoms that cannot be cured. Your doctor or therapist can be your partner in putting together an effective treatment and management plan.
Treatment for incontinence involves good communication with your doctor and/or your therapist so you both understand:
- How the disorder is affecting your daily life
- What is the underlying cause
- Factors that bring on an episode of incontinence or makes it worse
Constipation and diarrhea are common causes that often can be managed. Your doctor or therapist may ask you to keep a diary for a couple of weeks of what you eat and drink. What you do or do not eat and drink can affect how often your bowels move and how hard or loose your stools are. For example, some foods are normally gas-producing.
It is important to learn what foods or drinks affect your bowels so that you can take in more of those that help, and less of those that cause you problems. Your doctor or a registered dietician can help adjust your diet.
Download IFFGD’s free personal daily diary
Bowel retraining works by teaching new skills to develop a regular and predictable schedule for evacuation. This helps decrease unpredictable bowel movements. Doctors, nurses, or therapists who are skilled in treating disorders of the colon or rectum can help you with this. The bowel retraining will include methods, and sometimes medicines, to help normalize stool consistency so the stool is formed (neither too hard nor too soft), and to establish and stimulate a regular time for having a bowel movement.
Read more about bowel training
No matter what the cause of incontinence, dietary and bowel retraining measures can often help. Additional treatment may be needed if nerves or muscles in the pelvic floor area are not working properly.
Biofeedback is a painless therapy that uses special sensors and a video screen to help improve the nerve sensation and muscle control that is needed to control bowel movements. Working with a therapist skilled in using biofeedback for disorders of the pelvic floor and rectum can help you improve your ability to sense contents in the rectum and to hold in the contents.
Other newer procedures are being developed to treat incontinence. These range from electrical stimulation to implants to injections. If muscle is damaged but nerves are functioning, surgery is sometimes suggested. Another option some people choose when other treatments fail is to have a colostomy; this involves a surgical procedure to divert stool to a pouch outside the body.
Be sure to talk to your doctor about all options, possible risks, and chances of success. Think about what “success” means to you. Does it mean cure; or does it mean managing symptoms so you can get on with your life? A cure may not be possible. Treatments may have their own set of side effects. It is important that you understand your options and work with your doctor or therapist to set your own treatment goals.
Putting it all together
Incontinence is a symptom – a sign that something is wrong. Treatment may improve but not always cure the symptom. There are ways to help manage incontinence. The first step is to recognize that something is wrong and seek help.
Doctors do not receive much training about bowel incontinence in medical schools, and no type of doctor specializes in treating bowel incontinence. Start with your primary care physician.
It is important that when you talk to a doctor about your incontinence he or she respond to you with interest and concern. If that does not happen, we suggest you find another doctor. Your doctor may not have all the answers – much remains to be learned about the condition – but he or she should listen to you and work with you to find existing solutions that work best for you.
Adapted from IFFGD Publication: Bowel Incontinence and Aging by William F. Norton, Publications Editor, IFFGD, Milwaukee, WI; and Jeannette Tries, PhD, Director of Therapy Services, Aurora Women’s Pavilion of West Allis Memorial Hospital, WI, and Director of Biofeedback Services, Continence Control Service, University of Illinois, Chicago, IL.









