Introduction
Cancer of the colon and rectum remains one of the most deadly forms of cancer. It is the third most common cancer in the United States, yet it is quite curable by surgery when found in its early stages.
Since it involves the lower gastrointestinal tract, treatment of colon and rectal cancer frequently affects bowel function and, at times, continence. Colorectal cancer therapy, both surgical and medical, may affect bowel continence.
What is Continence?
Bowel continence is the ability to delay having a bowel movement in a controlled manner. Continence is complex. It involves the way the body functions (physiology), anatomy, sensation, and awareness or thinking (cognition).
In the normal healthy adult, the small intestine transfers liquid stool to the colon (large intestine/bowel).
The colon then absorbs liquid in the stool until the stool reaches the rectum. The rectum is the last part of the colon and is about 6 inches long. The rectum can expand to hold stool. It ends at the anus. (figure1) Muscles (internal and external anal sphincters), sensory nerves, lubricating glands, and a complex blood supply make the anus one of the most complex and sophisticated parts of the body.
A bowel movement (defecation) occurs when the rectum becomes expanded with stool. This causes the internal anal sphincter to relax. The anal canal detects whether there is gas, liquid or solid matter present. The brain receives this information and decides whether to pass the rectal contents or not.
To allow passage of the stool, the external sphincter muscle along with other pelvic floor muscles may be voluntarily relaxed. The diaphragm and abdominal muscles bear down, increasing the pressure on the so the stool passes through the anal canal.
Continence thus depends on:
- Volume and consistency of stool
- Capacity and function of the colon and rectum
- Function of the internal and external sphincters
- Sensory function of the rectum and anal canal
- Motor function of the sphincter muscles and pelvic floor muscles
- Cognitive function
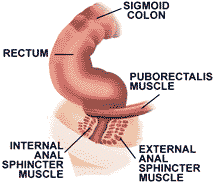
Figure 1. Anatomy of the Rectum and Anal Canal
Colon and Rectal Cancer: Basic Concepts
Treatment of cancer may impact many of the factors affecting continence. Colon and rectal cancers arise from the inner lining of the bowel, known as the mucosa. Cancers develop when changes, or mutations, occur in a series of genes that control cell growth. These changes allow mucosal cells to grow rapidly and in an uncontrolled manner.
The abnormal cells often look different than normal cells when examined under a microscope – this is called dysplasia. As these cells multiply, they form abnormal structures called polyps. A polyp is an overgrowth of the mucosal lining, which may be seen during endoscopy. Often, they may be removed with the colonoscope and then they will not develop into a cancer.
Colonoscopy
Colonoscopy is a fiber optic (endoscopic) procedure in which a thin, flexible, lighted viewing tube (a colonoscope) is threaded up through the rectum for the purpose of inspecting the entire colon and rectum. If there is an abnormality, it will be examined or removed.
With time and additional changes in the genes, the cells acquire the ability grow into the deeper muscular walls of the intestine. Once this mass of cells, now called a tumor, invades the deeper bowel wall, it is called a cancer because it has demonstrated the ability to spread.
Invasion into adjacent tissues and spread to the regional lymph nodes located in tissue next to the intestine, called the mesentery, are the hallmarks of colorectal cancer. Cancer cells may further spread though the lymphatic channels and the blood stream to distant sites including the liver, lungs, and other parts of the body. This process is called metastasis.
Cancer located within the inner wall of the colon is considered Stage I. If removed (resected) surgically at this point there is a 90% five year survival rate and no additional therapy is needed.
As cancer progresses, survival rates decrease.
Cancers that penetrate more deeply into the wall or into surrounding tissues are considered Stage II.
When there is cancer detected in the lymph nodes in the mesentery, the cancer is considered Stage III.
When cancer has spread to other organs such as the liver or lungs, it is considered Stage IV and usually not curable. Selected patients with limited disease in the liver or lungs may be cured with additional surgery.
Adjuvant therapy is treatment used in addition to surgery and denotes the use of either chemotherapy or radiation therapy or both.
Chemotherapy using drugs designed to destroy cancer cells has been shown to prolong life in both Stage III and Stage IV colorectal cancer.
Radiation therapy is used primarily for patients with rectal cancer. It may both increase survival and decrease the rate of local recurrence of the tumor in the pelvis where the rectum was removed.
The first step in treating a person with colorectal cancer is to determine if the cancer has spread or not. Treatment may then be recommended to attempt a cure. If the cancer has spread widely, therapy aims to relieve or prevent symptoms, slow the progression of disease, and maintain quality of life.
Continence and Colon Cancer
Treatment of colon cancer rarely results in permanent incontinence (loss of bowel control; accidental leakage or seepage). When a segment of the colon is removed, the length of colon available to absorb fluid is reduced. Thus, stools may be more liquid. Generally, this returns to normal over time.
However, if the liquid stool volume is too high for the remaining colon to handle, a large amount of liquid will fill the rectum. This may overwhelm both the rectal storage capacity and the sphincter muscle tone. Certain chemotherapy drugs may worsen this problem by causing significant diarrhea due to their effects on both normal and cancerous tissues.
If the person was continent prior to surgery and did not have any injury to or surgery on the anal sphincter muscles, incontinence should be limited and eventually improve.
Continence and Rectal Cancer
Treatment of rectal cancer often directly affects continence. Preservation of continence in the person with rectal cancer poses several challenges.
Continence is put at risk by a number of factors:
- Position of the cancer low in the rectum
- Affect on the anal sphincters
- Surgical technique applied
- Use of radiation
Radiation Effects
Radiation is often used to treat pelvic cancers with or without surgery. Radiation kills rapidly dividing cells in its path, which include cancer cells but also mucosal cells.
In the short term, radiation causes injury to the lining of the rectum, vagina, and bladder and can result in inflammation and ulcers. The rectal effects are termed early radiation proctitis. Late radiation proctitis symptoms result from scarring of the rectal and anal muscles. Patients can experience frequent bowel movement, urgency, bleeding, and incontinence.
Treatment of radiation proctitis includes all the methods listed below as well as direct treatment of bleeding sites.
Learn more about treating radiation proctitis
Treatment for Incontinence
Initial therapy includes bowel management and dietary changes. The use of dietary fiber, fluids, a regulated diet, and scheduled meals help to make bowel movements predictable. Local care using pads, barrier agents, frequent baths, and clothing changes help to protect the perianal skin and lessen the impact of incontinence episodes.
Learn more about managing incontinence
The next step is to add antidiarrheal agents such as Imodium and Lomotil that decrease the frequency and volume of bowel movements. Daily rectal cleansing enemas [as directed by your physician] may stimulate bowel movements on a scheduled basis.
Learn more about medical management of incontinence
Biofeedback therapy, which improves rectal sensation, sphincter strength and muscle coordination, also often helps.
Further treatment is generally based in anorectal physiologic evaluation. Various surgical options are available. Bowel incontinence may be resolved by a colostomy or ileostomy; careful consideration of risks as well as benefit is advised.
Learn more about surgical treatment for incontinence
Conclusion
The primary goal of the treatment of colon and rectal cancer is to cure the disease. However, preservation of continence is an important additional consideration.
Most patients will be treated surgically and will have good to excellent bowel function afterwards. Before undergoing surgical therapy for colon and rectal cancer it is important to understand the overall plan as well as the risks and benefits.
When the cancer arises in the rectum, changes in bowel function are likely, due to surgical changes as well as the effects of adjuvant chemotherapy and radiation.
Evaluation by a specialist in the areas of colorectal cancer and bowel incontinence is often useful if initial treatment attempts are not helpful. Treatment options for incontinence include diet, medications, bowel management, biofeedback, surgery, or diversion. Function often improves over time.
Additional information is available from:
American Society of Colon and Rectal Surgeons, www.fascrs.org. The American Society of Colon and Rectal Surgeons is the leading professional society representing more than 1000 board certified Colon and Rectal surgeons and other surgeons dedicated to advancing and promoting the science and practice of the treatment of patients with diseases and disorders affecting the colon, rectum, and anus.
Adapted from IFFGD Publication: Colorectal Cancer and Continence by Joshua A. Katz, MD, and Bruce A. Orkin, MD, Division of Colon and Rectal Surgery, The George Washington University, Washington, DC.
